
At the 18th World Congress on Skin Cancer in Buenos Aires, Oct. 26-29, 2022 (https://wccs2022.com), Prof. Claus Garbe, M.D., of Tübingen, Germany, gave a keynote lecture on Obstacles to Melanoma Prevention (Why It Doesn’t Work). Garbe focused on incidence data for malignant melanoma in Europe, Denmark and Germany, compared with current hot spots in Australia and New Zealand at 50– 80 cases per 100,0001. While incidence curves are flattening in AUS and NZL, projections show that incidence levels in DEN and GER could reach similar levels by 2040; incredibly. Clearly, something is going hugely wrong in Europe, while AUS/ NZL seems to be reversing the trend in this important public health statistic.
Prof. Garbe’s conclusion was not only that sunscreens do not work, but worse yet that “the use of sunscreens promotes the development of skin cancer”. His conclusion is based on five statements:
- Even very low doses of UV radiation cause mutations in the skin (0.1– 0.2 MED).
- With intentional UV exposure, sunscreens do not prevent the development of melanocytic nevi
- The sun protection factor and the real protection factor differ by a factor 5– 10
- Sunscreens significantly prolong the stay in the sun
- In the last decades there is no evidence of prevention of melanoma in Europe
There is a lot to unpack in Garbe’s melanoma statistics, statements and conclusions. Obviously, there is a problem that is far from being solved in Europe, although solutions seem to exist in Australia/New Zealand. His first point is somewhat trivial, 0.1– 0.2 MED is a very low dose that one can get sooner or later, without or with sunscreen, the DNA repair system of a healthy person can easily cope. Garbe’s points 2 and 3 relate directly to the sunscreen and its proper application to the skin. The measured SPF should not be directly interpreted as a protection factor against melanoma, not even as a protection factor against erythema under outdoor conditions2. The fourth goes back to Autier P., who spoke many years ago of “sunscreen abuse for intentional sun exposure”3. The key word here is “abuse”. Misuse is never really helpful, but we must keep in mind that the purpose of sunscreens is, of course, protection from sun exposure, intentional or not, what else? The last point is a matter of epidemiology. Figure 1 shows data from a relatively recent review by Silva ESD et al between 1970 and 20104. Until the 1990s, the cumulative odds ratio for melanoma in the presence of sunscreen was greater than one (>1), implying that sunscreen use was associated with a higher risk. The use of weak sunscreens at that time was an indicator of high sun exposure rather than a protective measure against melanoma. But that has apparently changed, and we no longer see this phenomenon, although no protective effect is yet evident either. We can count this observation as a success in the use of sunscreens. In the last thirty years, sunscreens have improved considerably. In addition to higher SPF values, UVA protection in particular has improved significantly since the first UVA filter, avobenzone, became available around 1990. Today, we know that UVA radiation is a risk factor for the development of malignant melanoma, as noted in a recent article by Diane Godar: “The main risk factors for cutaneous malignant melanoma appear to be light hair color, especially red and white hair (reactive oxygen species and UVA; 320-400 nm), low cutaneous vitamin D3 levels, and post-1960 human papillomavirus, whereas there was no apparent risk from UVB exposure (290-320 nm) or sunburns”5.
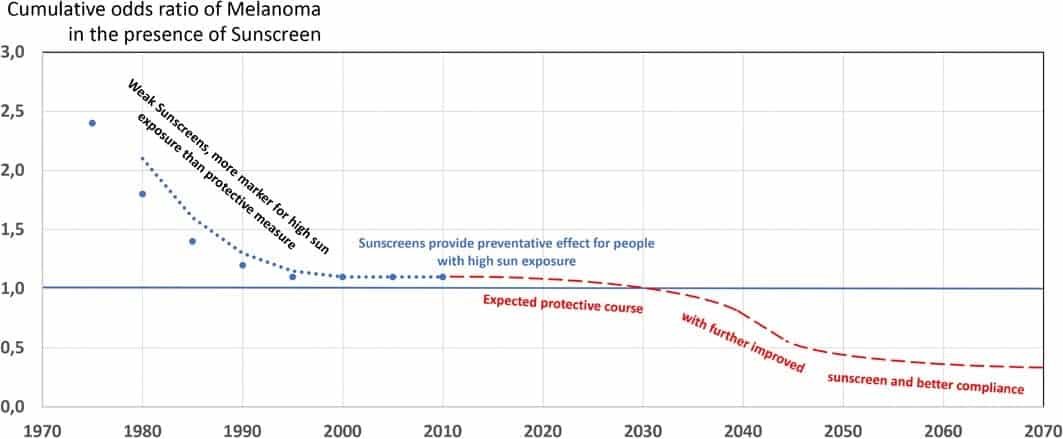
Two factors need to continue to improve before we see a protective effect at the epidemiologic level: 1) sunscreens, particularly UVA protection and 2) compliance with sunscreen use. The latter has to do with the photo-education practiced in AUS/ NZL, i.e., all sun protection measures must be included, but also with the cosmetic acceptability of the sunscreen. Only sunscreens that people like to apply have a chance of providing long-term protection. However, decades will pass before this effect will be seen (Figure 1).
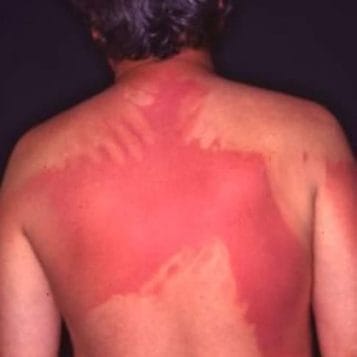
But that doesn’t mean we have to wait decades to protect ourselves properly with sunscreens. We know from experience that sunscreens work when used properly. There is no doubt that sunscreens work against sunburn (erythema). Figure 2 shows this impressively, and only where sunscreens have been properly applied to the skin. But what about protection against skin aging and skin cancer? The landmark study conducted in Australia in the late 1990s by Adele Green et al. showed that sunscreens have a protective effect against squamous cell skin cancer6, malignant melanoma7, and also against skin aging8. The study was often criticized because it showed barely significant results. However, we must remember that the sunscreen was SPF 16 and contained two UV filters, octinoxate for UVB and avobenzone for UVA, and we now know that this combination is not photostable. Also, for obvious ethical reasons, there was no real (negative) control group. Participants in the control group could use whatever they wanted, even though there were no good sunscreens available yet and the Australian UVA standard had just been introduced.
Prof. Garbe presented an interesting study of 1812 children aged 2–7 years that examined the protective effect of clothing based on the development of childhood melanocytic nevi, which are associated with melanoma. In contrast to the use of sunscreens, covering with a T-shirt, shorts, and cap had a significant or highly significant protective effect9.
So, we know that covering-up works, i.e., uniform protection across the entire UV range, even in the visible range. Thus, in my presentation The Future of Sunscreens toward the end of the Buenos Aires Congress, I concluded that the protective profile of sunscreens should be similar to the profile of clothing. Such uniform protection is also known as “spectral homeostasis protection,” first proposed by Diffey in 1991. Today, it is possible to formulate sunscreens that closely approximate the optimal uniform protection profile10.
In addition, new UV filters are coming onto the market that cover the long UVA range up to 400 nm, and some extend beyond that into the visible range: Phenylene bis-diphenyltriazine (Tri- AsorB, PIERRE FABRE), Methoxypropylamino cyclohexenylidene ethoxyethylcyanoacetate (Mexoryl 400, L’ORÉAL) and Bis- (diethylaminohydroxybenzoylbenzoyl) piperazine (NANO) (HAA299, BASF). This is confirmation that the industry is on the right track with UV filters. The exception, of course, is the USA, where none of the modern UVA and broad-spectrum filters have so far been approved by the FDA. On the other hand, based on the studies by Green et al 6–8, the FDA recognizes that “sunscreens help prevent skin cancer and skin aging.” Because sunscreens are effective when used properly, individuals need to take care to protect themselves adequately and not misuse sunscreens.
References:
- Garbe C, Keim U, Gandini S, Amaral T, Katalinic A, Hollezcek B, Martus P, Flatz L, Leiter U, Whiteman D. Epidemiology of cutaneous melanoma and keratinocyte cancer in white populations 1943-2036. Eur J Cancer. 2021 Jul;152:18-25. doi: 10.1016/j.ejca.2021.04.029. Epub 2021 May 29. PMID: 34062483
- Diffey B, Osterwalder U. Labelled sunscreen SPFs may overestimate protection in natural sunlight. Photochem Photobiol Sci. 2017 Oct 11;16(10):1519-1523. doi: 10.1039/c7pp00260b. PMID: 28812776.
- Autier P. Sunscreen abuse for intentional sun exposure. Br J Dermatol. 2009 Nov;161 Suppl 3:40-5. doi: 10.1111/j.1365-2133.2009.09448.x. PMID: 19775356
- Silva ESD, Tavares R, Paulitsch FDS, Zhang L. Use of sunscreen and risk of melanoma and non-mel- anoma skin cancer: a systematic review and metaanalysis. Eur J Dermatol. 2018;28(2):186–201. doi: 10.1684/ejd.2018.3251
- Godar DE. UV and Reactive Oxygen Species Activate Human Papillomaviruses Causing Skin Cancers. Curr Probl Dermatol. 2021;55:339-353. doi: 10.1159/000517643. Epub 2021 Oct 25. PMID: 34698023
- Green A, Williams G, Neale R, Hart V, Leslie D, Parsons P, et al. Daily sunscreen application and betacarotene supplementation in prevention of basalcell and squamous-cell carcinomas of the skin: a randomized controlled trial Lancet. 1999;354(9180):723–9. doi: 10.1016/s0140-6736(98)12168-2
- Green AC, Williams GM, Logan V, Strutton GM. Reduced melanoma after regular sunscreen use: rand- omized trial follow-up. J Clin Oncol. 2011;29(3): 257–63. doi: 10.1200/jco.2010.28.7078
- Hughes MCB, Williams GM, Baker P, Green AC. Sunscreen and prevention of skin aging: a randomized trial. Ann Intern Med. 2013;158(11):781–90. doi: 10.7326/0003 4819-158-11-201306040-00002
- Bauer J, Büttner P, Wiecker TS, Luther H, Garbe C. Effect of sunscreen and clothing on the num- ber of melanocytic nevi in 1,812 German children attending day care. Am J Epidemiol. 2005 Apr 1;161(7):620-7. doi: 10.1093/aje/kwi086. PMID: 15781951
- Dudley DK, Laughlin SA, Osterwalder U. Spectral Homeostasis – The Fundamental Requirement for an Ideal Sunscreen. Curr Probl Dermatol. 2021;55:72-92. doi: 10.1159/000517593. Epub 2021 Oct 25. PMID: 34698022

Uli Osterwalder
Uli Osterwalder studied Chemical Engineering at ETH Zurich, Switzerland and at the University of Houston in Houston, Texas. He joined Ciba-Geigy in Basel in 1979 where he first developed a Phosgene Generator in central process development. Later he developed his leadership skills in Project Management and Process Analytics. At Ciba Specialty Chemicals Uli Osterwalder helped establish new business development in Fabric Care and Personal Care. After the acquisition by BASF SE he became Senior Marketing Manager and Scientific Adviser in Sun Care in Ludwigshafen and Duesseldorf.
2016 he came back to Basel, working for DSM as senior Senior Scientific Adviser suncare for two years. 2018 he started his own company, Sun Protection Facilitator GmbH and is committed to contribute to further improvements in sun protection. Uli Osterwalder works for ISO on the development of new UV protection assessment methods and is now chairing the technical committee ISO TC/217 (Cosmetics). He is author and co-author of numerous scientific articles and book chapters on sun protection.



